Prairie healthcare: long waits, staffing shortages and eroding trust
A growing number of residents in Saskatchewan and Manitoba say they are losing confidence in the public healthcare system, according to responses from The Flatlander’s recent survey.
Across hundreds of responses, many described a system defined by long waits, staff shortages and increasing barriers to accessing care, challenges that, for some, have had life-altering consequences.
A system of waiting and then waiting again
For many respondents, accessing care involves not one wait, but several.
Local, independent, in-depth.
Our Prairie stories.
Patients described waiting months for diagnostic tests such as MRIs and CT scans, delays that can prevent them from being placed on surgical waitlists. This “pre-wait” phase, as some respondents described it, has become a significant bottleneck in the system.
In some cases, those delays have had lasting consequences.
One respondent from Yorkton, Saskatchewan, said they waited four months to see a specialist after fracturing two vertebrae. By the time they were assessed, the bones had “healed crooked,” leaving them with permanent pain.
Others described waits that ended in tragedy.
In rural Ste-Geneviève, Manitoba, one respondent said their wife died after waiting more than 30 minutes for paramedics to arrive. In the Rural Municipality of North Qu’Appelle, Saskatchewan, another respondent reported waiting 45 minutes for an ambulance while their husband was dying at home.
Paying to bypass the system
Faced with long delays, some residents say they are turning to private care, often at significant personal expense.
Respondents from Regina and Prince Albert reported travelling to Calgary or the United States and paying more than $1,400 out of pocket for private MRIs.
“I’ve had to pay for private healthcare rather than risking him dying,” one Regina resident wrote of a family member. “It’s terrible in Saskatchewan.”
The trend reflects growing concern that access to timely care is increasingly tied to a patient’s ability to pay.
Staff shortages and the ‘agency nurse’ dilemma
Staffing shortages were another recurring theme.
Respondents pointed to a system struggling to retain permanent staff while relying heavily on temporary, or “agency,” nurses, a practice some described as both costly and demoralizing.
Agency nurses can cost significantly more than permanent employees, sometimes several times higher, according to respondents. Some said temporary staff often have limited patient interaction and no long-term connection to the communities they serve.
A respondent from Crystal City, Manitoba, described frustration with what they saw as an imbalance in workload and compensation, with local staff carrying the burden of complex care.
Both Saskatchewan and Manitoba have indicated they are working to reduce reliance on agency nurses. However, local staffing shortages make it difficult to fully replace them, creating a “catch-22.”
Communities paying the price, twice
In some areas, residents say the strain on the health system is being felt locally and financially.
In Kindersley, Saskatchewan, residents have raised funds to purchase medical equipment and even repair hospital infrastructure, including most recently, a parking lot. The regional health authority did not contribute to the project.
Such efforts have led some to question whether they are effectively paying twice: once through taxes, and again through community fundraising.
A growing shortage of family doctors
Many respondents also described difficulty accessing primary care, pointing to what some called a “succession crisis” among family physicians.
In Brandon, Manitoba, one respondent said they had seen the same doctor for 34 years. When that doctor died in 2024, they were placed on a waiting list for a new physician and now rely on emergency rooms for routine care.
Others described a pattern of short-term placements in smaller communities, where physicians stay only a few years before leaving, forcing patients to repeatedly start over with new providers.
“Just when you feel comfortable with a doctor, they move on,” one respondent wrote.
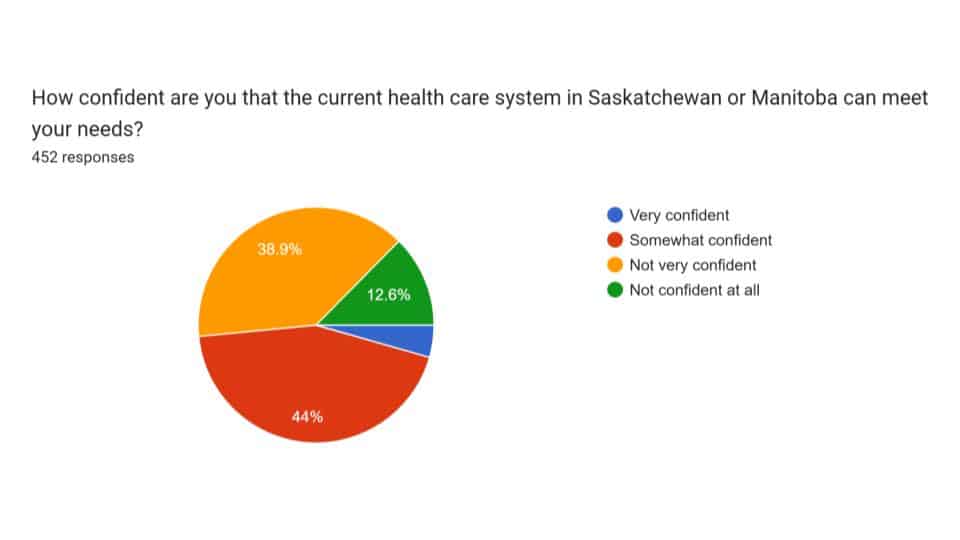
Confidence in the system is declining
Taken together, the responses point to a broader erosion of trust.
A majority of respondents across both provinces said they were “not very confident” or “not confident at all” that the healthcare system could meet their needs.
At the same time, many were careful to distinguish between the system itself and the people working within it.
Frontline workers, such as nurses, paramedics, doctors and support staff, were frequently praised for their efforts under difficult conditions.
The frustration, respondents said, is directed not at those providing care, but at the systems struggling to support them.
Read more:

We asked about healthcare. The answers were honest.
What happens when hundreds of Prairie residents compare notes on healthcare? A story emerges of waiting, missing doctors, long drives for care and growing frustration. Read more.
Hallway medicine and questions about system capacity
Some respondents described what is often referred to as “hallway medicine,” where patients remain on stretchers in emergency department corridors due to a lack of available beds.
While frontline staffing shortages were a consistent concern, some respondents also questioned whether administrative structures are contributing to the strain. One Regina respondent asked how many layers of management exist within the system, suggesting resources may not be reaching the front lines where they are most needed.
For patients, the consequences can be severe.
A respondent from Cudworth described a friend with advanced cancer who was forced to relocate to Saskatoon because no hospital beds were available closer to home.
At one point, the patient was placed on a stretcher in a storage room for several days.
“She was quietly dying,” the respondent wrote. “But there just weren’t enough beds.”
Concerns about the role of private care
Some respondents raised concerns about the growing role of private health services, suggesting that long wait times and staffing shortages may be contributing to a gradual shift away from public care.
“I believe that the biggest issue is the deliberate slow creep of private healthcare eroding our system,” one Regina respondent wrote.
Others questioned whether persistent recruitment and retention challenges are unintentionally, or deliberately, weakening the public system.
The perception, among some respondents, is that the current trajectory risks creating a two-tier system, where access to timely care increasingly depends on the ability to pay.
Our Prairie stories matter too.
The Flatlander takes a closer look at the stories that unite us, and make us unique, in Saskatchewan and Manitoba.
Will you help us tell our stories?



